Blood Disorders in Children: Common Types Every Parent Should Know
When we think about children’s health, we often focus on infections or growth. But sometimes, the issue lies deeper in the blood.
Blood disorders in children can affect how the body carries oxygen, fights infection, or controls bleeding.
What Are Blood Disorders?
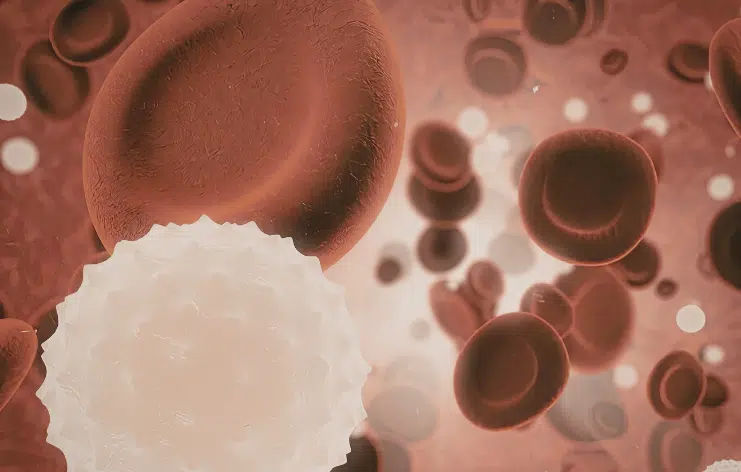
Blood disorders are conditions that affect:
- Red blood cells (carry oxygen)
- White blood cells (fight infections)
- Platelets (help in clotting)
Each plays a vital role in your child’s health.
Common Types Seen in Children
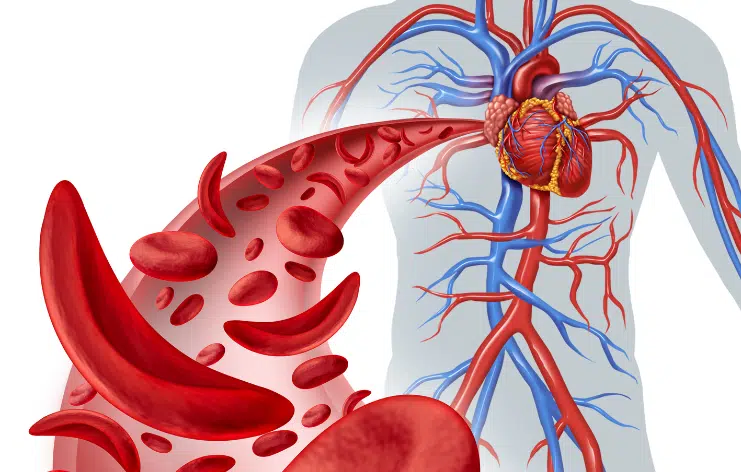
Some of the more common blood-related conditions include:
- Anemia – Low red blood cells leading to fatigue
- Thalassemia – A genetic condition affecting hemoglobin
- Sickle Cell Disease – Abnormal red blood cell shape
- Platelet Disorders – Leading to easy bruising or bleeding
- Leukemia – A type of blood cancer
Signs Parents Should Notice
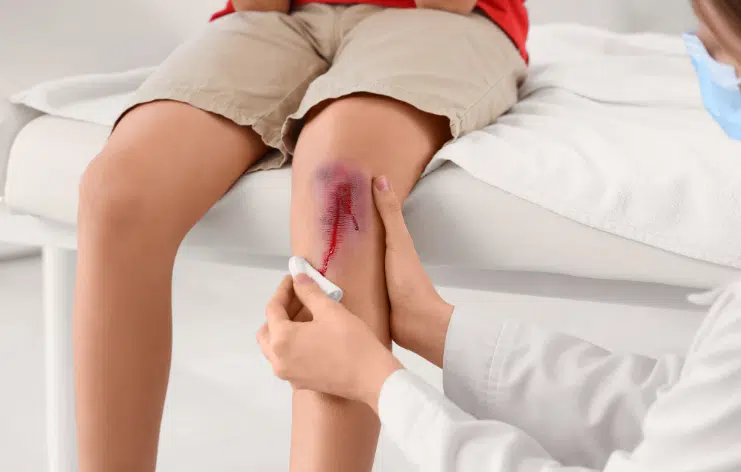
- Frequent infections
- Easy bruising or bleeding
- Delayed growth or weakness
These symptoms may seem mild at firstbut they deserve attention if persistent.
Why Early Diagnosis Matters
Many blood disorders are manageableand some are treatable when identified early.
Delays can lead to complications, but timely care improves outcomes significantly.
What Parents Can Do
- Don’t ignore persistent fatigue
- Follow up on abnormal blood reports
- Seek specialist advice when needed
Frequently Asked Questions:
1. Are blood disorders serious?
Some are mild, others need long-term carebut early diagnosis helps.
2. Can they be treated?
Yes, many conditions are manageable with proper care.
3. Are they genetic?
Some are inherited, others develop over time.
For expert evaluation and care, consult our pediatric hematology specialists.